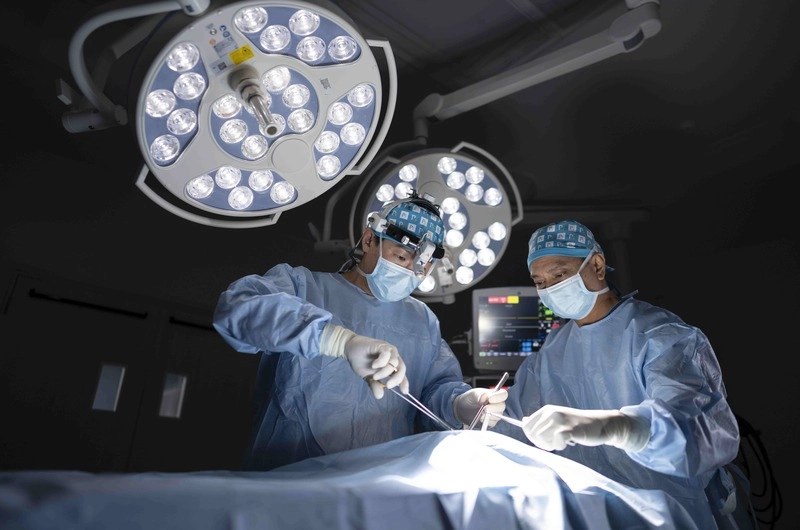
Is This Endometriosis? The Symptoms You Shouldn’t Ignore
March 25, 2026
Because period pain should not steal your life.
Many women grow up believing that pain is simply “part of being a woman.” Pain during menstruation is often normalised, brushed aside, or even joked about—until one day it becomes unbearable.
But there is a difference between mild period discomfort and pain that signals that something deeper may be happening inside the pelvis.
One of the most common reasons nearly 10% of young women worldwide suffer silently for years is endometriosis—a condition that can affect not only the womb, but also the ovaries, bowel, bladder, pelvic nerves, and surrounding tissues. It is also one of the most misunderstood conditions in women’s health, and is often ignored.

What is Endometriosis?
Endometriosis happens when tissue similar to the lining of the uterus (the endometrium) grows outside the uterus, where it does not belong. This triggers chronic inflammation and can lead to long-term complications.
This tissue can be found on the ovaries, fallopian tubes, pelvic peritoneum (the lining inside the pelvis), bowel and rectum, bladder, ureters (the tubes that carry urine from the kidneys), deeper pelvic ligaments and nerves, and in rare cases, even areas beyond the pelvis.
As a result of repeated inflammation that flares up during each menstrual cycle, endometriosis may eventually lead to:
- scarring and adhesions (pelvic organs sticking together)
- ovarian endometriomas (“chocolate cysts”)
- debilitating pain that worsens over time
- fertility challenges in some women
Endometriosis is not “just a bad period.” It is a real medical condition, and it deserves proper attention If left untreated, deeply infiltrating endometriosis can lead to serious complications such as intestinal obstruction, ureteric stenosis, hydronephrosis, and kidney damage. According to the literature, about 1–3% of endometriosis cases may undergo malignant (cancerous) transformation.
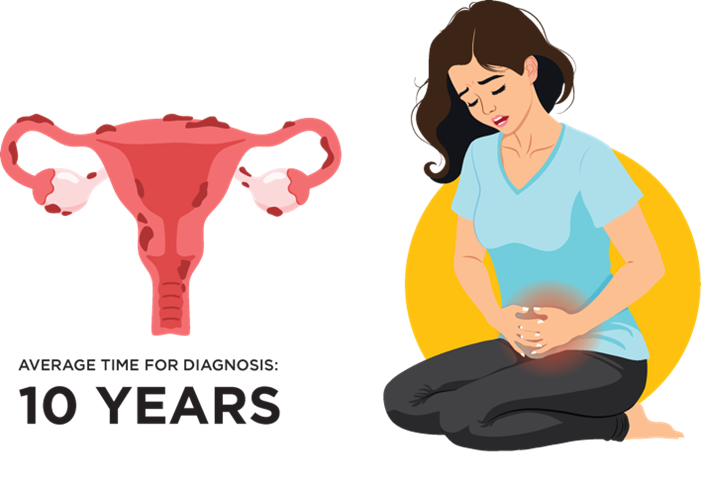
How Do You Know When Your Period Pain is NOT Normal?
Many women experience mild cramps on the first day of their period. This is common.
However, pain should never:
- stop you from going to school or work
- make you faint, vomit, or feel paralysed
- require repeated visits to the emergency department
- require strong painkillers every month
- worsen year after year
- affect your mental health and relationships
Key Symptoms of Endometriosis You Shouldn’t Ignore
Endometriosis can look different in every woman. Some have mild symptoms, while others suffer severely. The intensity of symptoms does not always match the “stage” of the disease.

Endometriosis may start early in adolescence, sometimes soon after the first period (menarche).
Here are the most common symptoms.
1) Painful Periods (Dysmenorrhoea) That Are Severe or Getting Worse
This is often the earliest symptom and is experienced by the majority of women with endometriosis.
You may notice cramps that:
- start days before the period begins
- last throughout the period
- persist even after the period ends
The pain may radiate to the lower back or thighs and can make it difficult to stand or walk properly.
2) Chronic Pelvic Pain (Pain Even When You’re Not Having Your Period)
Endometriosis pain does not always follow the calendar.
You may experience:
- persistent heaviness or aching in the pelvis
- random stabbing pains
- discomfort after standing too long
- pain after exercise
- pain that flares unpredictably
Many patients feel frustrated because they look “normal” on the outside—yet they are fighting pain every day.
3) Pain During Sex (Dyspareunia)
This is an important but sensitive symptom, and many women feel too embarrassed to bring it up.
Pain may occur:
- during deep penetration
- after intercourse (lasting hours or even days)
- as pelvic soreness that affects intimacy and confidence
Deep pain during sex can be linked to deep endometriosis, especially behind the uterus or involving pelvic ligaments.
4) Bowel Symptoms: Constipation, Painful Bowel Movements, or “IBS-like” Symptoms
Endometriosis is often misdiagnosed as “gastric” problems.
You may experience:
- constipation that worsens during menstruation
- painful bowel motion (dyschezia)
- bloating that makes you look “pregnant” (“endo belly”)
- cramps after eating
- alternating bowel habits (constipation and diarrhoea)
Some women are told they have Irritable Bowel Syndrome (IBS) and are treated for IBS for many years before finally being diagnosed with endometriosis.
IBS is real—but when bowel symptoms are closely tied to menstruation and pelvic pain, endometriosis must be considered.
5) Bladder Symptoms: Painful Urination or Frequent Urge
Endometriosis can affect areas near the bladder or ureters.
You may notice:
- pain during urination or after voiding, especially around menstruation
- frequent urge to urinate
- UTI-like symptoms, but urine tests keep coming back negative
It is not uncommon for many women to be repeatedly treated for urinary tract infection, only to later discover that the real cause is endometriosis.
6) Heavy Menstrual Bleeding and Clots
Not all women with endometriosis have heavy periods, but many do—especially those with co-existing conditions such as adenomyosis or uterine fibroids.
If you experience:
- soaking pads every hour or two
- passing large clots
- bleeding longer than 7 days
- fatigue or low iron (anaemia)
…do not assume it is normal.
You may also have adenomyosis, which often co-exists with endometriosis. Adenomyosis occurs when uterine lining tissue grows into the muscle wall of the uterus, causing:
- extremely painful and heavy bleeding
- an enlarged, tender uterus
7) Fatigue That Doesn’t Improve With Rest
Fatigue is one of the most overlooked symptoms.
This may be due to chronic inflammation that exhausts the body, poor sleep from pain, hormonal fluctuations, iron deficiency from heavy bleeding, or emotional stress from living with an invisible illness.
If your fatigue is persistent, it deserves evaluation—not dismissal. Endometriosis drains energy and can dampen the soul.
8) Fertility Challenges
According to many studies, about 45–50% of women with infertility may have endometriosis. However, many women with endometriosis do become pregnant naturally too, while others may require medical assistance.
Women with endometriosis who conceive may also have a higher risk of:
- miscarriage
- premature delivery
- poor obstetric outcomes
Endometriosis can reduce fertility due to:
- inflammation affecting egg quality
- adhesions distorting pelvic anatomy
- blocked fallopian tubes
- ovarian endometriomas affecting ovarian reserve
If you have been trying to conceive for 12 months (if age <35), or 6 months (if age ≥35), and you also have symptoms of endometriosis, do not wait. Early assessment can save time and emotional heartbreak.
Red Flags: When You Should Seek Help Early
If you have any of the following, it is strongly recommended to see a doctor with experience in endometriosis:
RED FLAGS
- 1 pain that makes you miss work or school every month
- 2 pain that worsens each year
- 3 pain requiring strong painkillers regularly
- 4 pain during sex
- 5 bowel/bladder symptoms linked to periods
- 6 persistent pelvic pain beyond menstruation
- 7 history of ovarian cysts or surgery
- 8 fertility concerns
- 9 previous surgery but pain returned quickly
How is Endometriosis Diagnosed?
Diagnosis depends on symptoms, examination, and imaging.
1) Clinical assessment
A detailed history often gives the strongest clue and based on this alone, the diagnosis can be made with almost 80% accuracy.
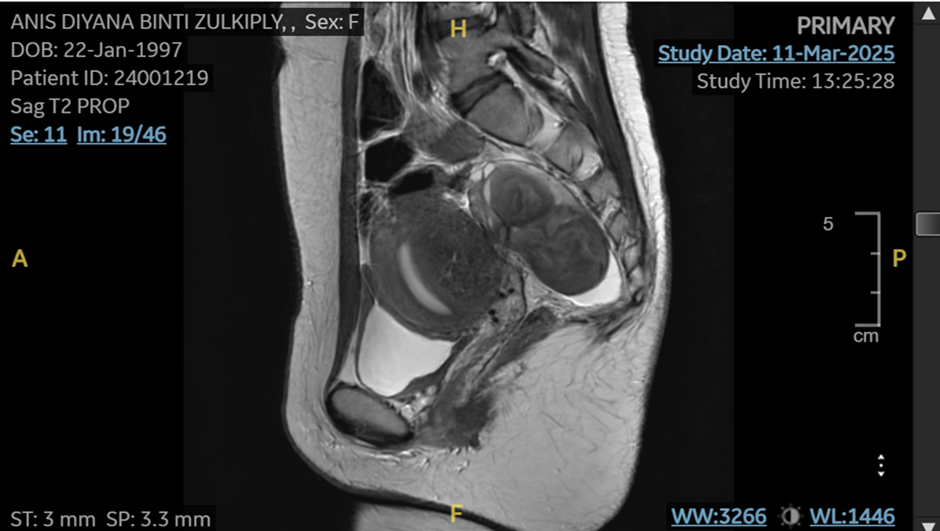
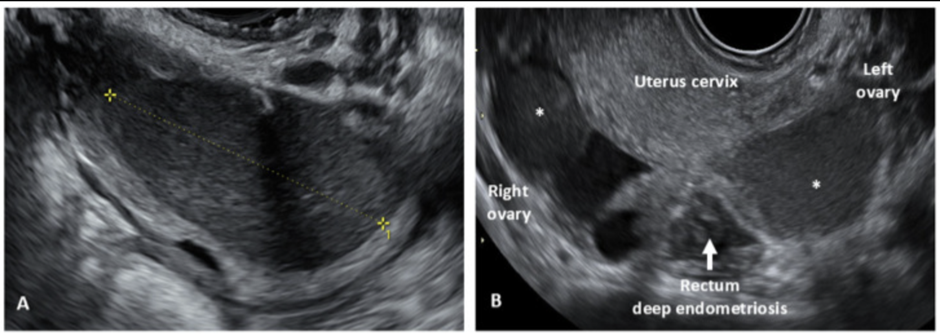
2) Ultrasound / MRI
Ultrasound of pelvis or MRI to diagnose and map the endometriosis are both equally accurate and useful. Specialised imaging can detect:
- endometriomas (chocolate cyst)
- the location of deep infiltrating endometriosis
- adenomyosis or fibroids
- pelvic adhesions and organ fixation
However, imaging requires both experience and the right technique. Not all general gynaecologists are trained in ultrasound to detect endometriosis, and not all radiologists are trained to interpret endometriosis accurately on MRI.
3) Laparoscopy (keyhole surgery)
Most endometriosis cases can be suspected and diagnosed accurately through clinical assessment and imaging. Treatment can often be initiated based on clinical diagnosis alone.
However, some women may require diagnostic laparoscopy for a definitive diagnosis and proper treatment.
Minimally invasive surgery may be recommended when:
- symptoms are severe
- medical treatment does not work
- fertility is affected
- deep disease is suspected
- diagnosis and treatment need to be done together
What Can You Do If You Suspect Endometriosis?
Here are simple steps you can start today:
1. Track your symptoms
Write down:
- pain score (0–10, no pain, 10 maximum pain)
- days of pain per month
- bowel/bladder symptoms
- triggers and relief methods
- bleeding pattern
If your pain score is consistently >6/10, it may suggest a significant underlying issue and should be assessed.
2. Stop normalising suffering
Pain is not your personality. You are not weak.
You are not “overreacting.”
You are listening to your body.
3. See the right team early
At Hospital Picaso, endometriosis care is delivered through a multidisciplinary team, bringing together gynaecologists and other specialists when needed. Coordinated care helps ensure accurate diagnosis, personalised treatment, and better long-term outcomes.
A Message to Every Woman Reading This
If your pain has been dismissed for years, please remember:
You deserve to be believed.
You deserve proper assessment.
You deserve a life beyond pain.
At Hospital Picaso, we believe that women should not only be treated—they should be heard, supported, and empowered.

By: Dr Sharifah Halimah Jaafar (Author of the book “Fighting The Devil Within”)
返回